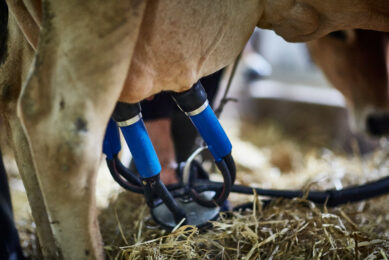
Timing: A top priority in E. coli induced mastitis
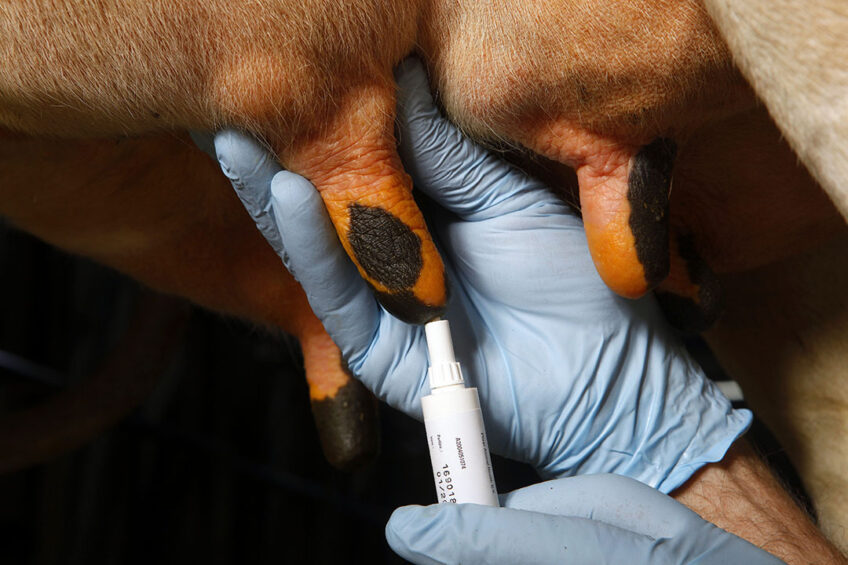
Cows infected with E. coli can get severely ill. Rapid intervention with supporting therapy should be a top priority.
Every livestock farmer has seen it at some point: a cow suddenly becoming critically ill due to severe mastitis. Even though there are several causes, an infection with Escherichia coli (E. coli) is often quickly considered. Intervention is imperative. How to go about this however, is a matter of discussion, especially when it comes to using antibiotics. One group of vets thinks that using antibiotics should be the standard, in accordance with the formulary for dairy cattle.

The formulary for dairy cattle
Bouwen Scheijgrond, board member of the KNMvD Commission Ruminants (the Dutch veterinary association) says: “The formulary prescribes antibiotics when a cow suffers from severe clinical mastitis.” He does add that the formulary is not a cookbook and that farmer and vet need to decide together how to handle the situation. Other vets do not feel that there is any added value to the currently available antibiotics. It is however certain that a severely ill cow needs immediate treatment. A bacteriological examination (BE) provides insight into what causes mastitis. Symptoms caused by E. coli, Klebsiella or sometimes even Staphylococcus aureus are similar. Even a severe form of infection by Staphylococcus uberis can cause the same clinical symptoms.
Timing is crucial for the cow’s survival chances.”
E. coli cannot always be determined with a BE, because the bacteria are often already dead and the toxins they excrete, are what make the cow particularly ill. Cultivation indicates the degree of the infection’s severity, because there is a connection between the numbers of coliforms and the severity of the illness. It is useful to know for future treatments if E. coli or other bacteria are involved. That is why a BE with a sensitivity test should be conducted.

More about E-coliEscherichia coli and Klebsiella are included among the environmental mastitis pathogens. E. coli is one of the most common mastitis pathogens. It thrives in bedding at temperatures of over 15˚C. E. coli is classified as a gram-negative bacterium, which mostly occurs in manure, free stalls and the soil. The route of infection is always external: bacteria enter the udder through the teat opening. Once inside the quarter, they can remain dormant, but they multiply explosively in most cases, producing toxins. Toxins are also released when the bacteria die, which literally causes critical illness in the cow. She runs a fever, loses appetite and the udder is painfully swollen and hard. Milk may contain flakes and clumps and, in some cases, even blood. The milk’s structure is watery and purulent. The cow can go into shock, which is very dangerous. When that happens, her chances of survival are reduced to only 20%. According to the VHS, about 95% of the mid-lactation cows that suffer from E. coli induced clinical mastitis is cured. Around calving, that percentage is reduced to only 10% to 15%. |
Biggest chance of survival
Christian Scherpenzeel, veterinarian and udder health expert at the Dutch Veterinary Health Service (VHS) says that an acutely ill cow always needs adequate treatment fast. “Timing is crucial for the cow’s survival chances. Always start with an urgent call to your vet. Then check the farm’s treatment plan for measures against severe clinical mastitis.” In this case, the cow is ill and runs a fever. Deviations to the milk and/or the udder occur.
“Only 5 to 10% of all clinical mastitis cases are severe and cause ‘intensive care patients,’” states Scherpenzeel. In these cases, it is justifiable to use a second-choice, broad-spectrum antibiotic that can also combat gram-negative bacteria, such as E. coli and Klebsiella.
Scheijgrond thinks that a severely ill cow should not be denied antibiotics. “Especially when the consideration involves keeping the daily dosage as low as possible.” Jan Dijkhuizen, cattle veterinarian at Graafschap Dierenartsen, is not convinced that using antibiotics immediately in case of E. coli induced mastitis is the right way to go about combating this pathogen. “The only antibiotics that were proven effective are third and fourth generation cephalosporins. The formulary prescribes Trimethoprim-Sulfa, but that is not enough for E. coli.”
Also interesting: New ‘cure’ to tackle mastitis
Supporting therapy
Scherpenzeel, Dijkhuizen and Scheijgrond all think that supporting therapy is more important than just antibiotics. “This treatment focuses on counteracting the toxins’ effects and prevents cows going into shock. Isolate the cow, preferably in a straw bedded pen, which makes the animal more comfortable. This also prevents pressure ulcers and subsequently, downer cows,” Scherpenzeel adds. In addition to this, it is important to use a non-steroidal inflammatory drug (NSAID). NSAID’s lower the animal’s temperature, are anti-inflammatory and reduce pain. Sometimes, under temperature occurs. In case of a direct fluid deficit, a cow shows visible signs of distress: her eyes are sunk back into her head, often in combination with cold ears. That is why you need to give water.

The vets also support using a calcium drip or a hypertonic drip for cows that have already gone into shock. The latter increases the salt content in the cow’s blood, attracting moisture to the vascular bed. This results in a stable blood pressure. It is important to maintain the fluid balance and thus the blood pressure. Only a vet is qualified to use a hypertonic drip. An adult, ill cow can certainly use 40 litres of lukewarm water through drenching, to supplement the extracted water from the surroundings of the vascular bed.
The VHS’s advice is to treat animals with severe clinical mastitis in accordance with the farm’s treatment plan, because an E. coli infection cannot be determined in advance. In addition to this, an E. coli infection can spread through the bloodstream. This means that sepsis occurs because of bacteria in the blood. Antibiotics that go through the bloodstream can thus be life-saving.
Also interesting: Image labelling to detect mastitis in cows
Chances of survival and prevention
Because E. coli is an environmental pathogen, prevention logically focuses on the cow’s surroundings.
|
Join 13,000+ subscribers
Subscribe to our newsletter to stay updated about all the need-to-know content in the dairy sector, two times a week.