New treatments for digital dermatitis
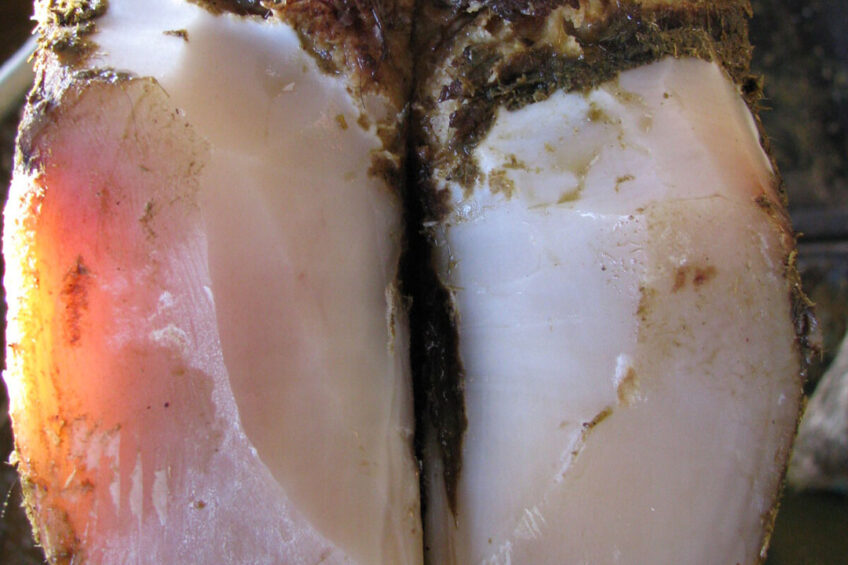
Whilst scientists and product developers still do not know all the details about the causal organisms of this persistent disease, treatments are evolving.
Digital dermatitis (DD), also called hairy heel warts, strawberry foot rot, raspberry heel, foot wart and hairy heel wart, is a globally recognised cause of dairy cow lameness. It was first discovered in Italy in the mid-1970s, arriving in North America and beyond in the years that followed.
A vaccine is not expected any time soon, and as dairy farmers well know, control of the disease is very difficult. Once established in a herd, digital dermatitis (DD) “typically becomes endemic,” noted a group of New Zealand scientists recently, “and very few herds are able to completely eradicate the disease due to the multifactorial and complex interactions between the bacteria, animal and environment.”
The results of their efforts to model DD transmission were published in February 2020, including a caution that in infected dairy herds, “on-going monitoring of DD is highly recommended.”

How the disease works
As Dr Anne-Sofie Vermeersch notes, “researchers possess some pieces of the ‘DD puzzle,’ but they still need to figure out how to put everything together in the right order. The presence of treponemes [one type of causal bacteria] is important, but we need to assess which role exactly they play.”
With her University of Gent (Belgium) veterinary school colleague Dr Geert Opsomer, Vermeersch recently published a 2-part overview of the factors contributing to DD development. They concluded that because current treatments are mainly directed against the treponemes and do not cure the disease, it’s therefore uncertain whether treponemes play the main role.
All the following factors – hygiene, bacteria, immunological mechanisms and genetic predisposition – and perhaps more contribute to the development of DD lesions, note Vermeersch and Opsomer, but the extent of each factors’ role and at which point it’s crucial in the disease process is yet to be discovered. It’s also not yet known how the disease spreads between cows and between farms, they note, but the leg and foot conformation of individual cows can affect susceptibility.
The immune system
Beyond leg/food conformation of a cow, genetics has been shown to play a role in DD in terms of immune system function. It was determined for example a few years ago that cows with a high level of antibody-mediated immune response (IR) had significantly lower prevalence of DD than cattle with an average or low IR. Conclusions of this research were eventually incorporated into the Immunity+ breeding platform owned by global genetics firm Semex.
Genomic programme manager at Semex Canada Dr Steven Larmer notes because cases of lameness in most commercial herds are not always well-characterised, he and his colleagues have grouped together all incidences of lameness in internal company studies. “We have seen in a study of 9500 genotyped cows from commercial herds a relative decrease in lameness of 39% in ‘High’ IR animals relative to their herdmates that tested either average or low [in IR],” he reports. “We know that DD is the primary infectious cause of lameness, and so we believe that decrease to mainly be decreased cases of DD.”
Dr Raphaël Guatteo, professor in Bovine Health Management at BIOEPAR-Oniris-INRA in France, notes that there is already, at least in that country, “the possibility to choose bulls with breeding index for infectious and non-infectious foot lesions.”
However, Vermeersch (whose research focus is the deviant response of the cow immune system) notes that “the first line of defence and further propagation of an immune response do not seem to protect the animal. Researchers have yet to discover why the lesions can become chronic or why a cow might relapse.”
Newest treatment strategies
After all this time, Vermeersch and Opsomer point out in their paper that knowledge of DD still “remains scarce,” and “without knowledge of the exact pathogenesis, it is challenging to establish an adequate, preventive and curative treatment.” Vermeersch adds that “lots of people tend to focus on giving supplements, but I think it is of crucial importance that the main feed ration is balanced correctly according to the needs of the herd/individual cows. There should not be any shortage or overabundance of certain elements in the feed ration.” Treatments – and prevention – for DD include foot baths and application of various products to the lesions. On the prevention front, Casey Jacobs at University of Calgary in Canada found in her recent Master’s thesis that no foot-bath protocol was superior to any other. For treatment, Jacobs found that routine use of commercially-available topical products was no more effective than saline in curing active lesions over 8 weeks.
In 2019, Guatteo and his colleagues published an analysis of how a new commercial biocide foot-bath product affected lesion healing, under different treatment regimens. In a trial with 1036 cows on dairy farms in western France, the scientists found the product to be effective when used in an intensive regimen. Use of this particular product also shortened time to healing in inactive lesions, but the scientists also point out that time to healing was delayed in feet that received hoof trimming in cows with a contralateral DD lesion, in cows in late lactation and in cows on farms with more than 100 cows. “These findings reinforce the crucial role of hygiene in DD dynamics and highlight the importance of implementing multiple control measures simultaneously,” states the team, “such as hygiene improvements in the barn, early detection and treatment of DD lesions and the correct usage of individual and collective treatments.”
Salicylic acid and more
Salicylic acid has been shown to be very effective for treating DD. It promotes removal of the epidermis and its low pH may also make it bacteriocidal. In 2019, several scientists in Germany published results comparing salicylic acid paste with polyurethane wound dressings for the treatment of active DD lesions and found both to be effective therapies.
Dr Andrea Fiedler, a veterinarian in Munich Germany, provides the following recommendations that she and her colleagues (Dr Katharina Grimm and Dr Charlotte Kröger) have found to provide impressive success in DD management, some of which involves salicylic acid. (Note first that DD lesions are classified according to size and other characteristics: M1 are active granulomatous area up to 2 cm, M2 are ulcerative lesion , M3 are lesions covered by a scab, M4 involved an chronic alteration of the skin, and M4.1 are lesions that are a combination of M4 and M1).
For M1 lesions, Fiedler recommends spray, preferably Repiderma but tetracyclin is also available. For M2 less than 1.5-2 cm, spray and cover with a bandage for 3 to 5 days. (All bandages should be the self-adhesive type and always have artificial cotton padding within. Fiedler also notes that whilst spray is seldom combined in European herds with a bandage, it always should be).
For M2 bigger than 1.5-2 cm (and also M3, M4 and M4.1 lesions), treatment should begin with Novaderma (containing 66% salicylic acid + methylsalicylat for pain) and a padded bandage for 5 days. This should be followed by spray and a bandage (again, with padding inside) for 5 more days. At that point, Novaderma should be applied again with a bandage and padding for 5 more days, if an alteration is still visible. (Alternatively for these types of lesions, apply spray with a polyurethane bandage for 14 days and repeat twice more, or apply Novaderma and a padded bandage for 5 days, then 2 14-day treatments of spray with a polyurethane bandage).
Microbe discovery needed
Going forward, Guatteo and colleagues state in their paper ‘Missing pieces of the puzzle’ to effectively control DD that “efforts to definitively determine the consortium of organisms necessary for DD disease induction should be a top priority.”
Although this will be costly and challenging, they note that “without knowing what specific bacterial organisms are necessary and sufficient for disease induction, all other efforts focused on better understanding organism ecology, immunity and treatment have the potential to focus on the wrong bacteria.”
References are available on request






